


One of my residents this morning thanked me for teaching her how to adjust the lights in the OR before a case. In fact, she said that since she had started this new practice that she hasn’t had to re-position the lights once while operating. There are so many minor details about the art of medicine that aren’t in books, so many things that make our lives easier…and that we wish someone had taught us earlier!
Operating Room Lights 101
Both lights should be positioned in the mid-line of the operative field – which means usually the mid-line of the table.
One of them should point straight down into the operative field. The second light should be either at the head or foot of the bed pointing into the field at an angle. If there are more than two, use them however it seems best.
Most importantly – You should position the lights BEFORE the procedure. Adjusting them after you start is always more difficult.
Operating Room Lights… Down the Historical Rabbit Hole
4500 BCE – Oil lamps
3000 BCE – Candles
1802 – Incandescent light invented by Humphrey Davy.
1850s – Operating rooms were built in the southeast corner on the top floor of hospitals to take advantage of natural sunlight. There were also four mirrors in the corners of the operating room to reflect sunlight toward the operating room table. (Wikipedia, Surgical Lighting).
1880s – Incandescent bulbs commercially available.
1920 – The scialytic (which means “dispersing or dispelling shadows”) light invented by Professor Verain in 1920 was the first design to direct light around the head of the surgeon. This allowed operating rooms to be moved from the top floor of hospitals. (Ersek, 1972)
1930s – Fluorescent lights commercially available
1962 – First LED light developed
“The light must be sufficient in quantity, must be directed into the proper places, and must be of such a quality that the pathological conditions are recognizable. Also the light cannot produce glare, which will serve to blind the surgeon, just as the high headlights of an oncoming automobile may incapacitate an automobile operator; and it is just as dangerous.” (Beck, 1971)
There are four factors to consider in optimizing illumination (reference)
Luminance = reflected light. Too much = glare = eye strain.
Volume. This refers to the need to have light in more than one plane, which is important because we operate in three dimensions (which is why there are always two lights). This is also why surgeons wear headlights or use lighted retractors.
Shadow management. This is why the position of the lights is important!
Temperature. Was much more of an issue before LED lights.
Setting the lights to set your intention
Positioning the lights before an operation will help you see more clearly. This simple act can also become a ritual and a reminder of why you are there… to heal.
Working as a surgeon for as long as I have, trust me, I have learned the agony and ecstasy of foot care. After a long case or after 24 hours on my feet it’s the agony. But I’ve learned how to make my feet happy… and I’ve learned that it’s not that hard.

Shoes
The ideal hospital shoe has a wide toe box, is flat, laced (I’ll get to clogs in a minute), lightweight, slip-resistant, fluid resistant, and can be thrown into the washing machine. You can expect to spend around $100 for these shoes. Don’t get cheap shoes – spend the money!
Although many running shoes meet these criteria, my current favorite shoe is from Merrell, which has been a go to company for me for years. The other major contender right now for favorite hospital shoe among medical students and residents is All-Birds.
Even though I wear lace up Merrells most days at work, I love clogs when I operate. They let me back my feet out of them and lower my heels to stretch my calves. I can kick them off and stand barefoot for a while if I need to change the pressure points on my feet. I had Dansko clogs for years, which are almost a tradition for surgeons, and then changed to Merrell clogs (which are pictured above) Although they are great for standing, the problem with clogs is that your toes have to grip the shoe when you walk (or run to a code), which means they aren’t the best shoes for the rest of your day.
Here are some other options beside running shoes, Merrells, and All-Birds to consider. If you have tried these or have other shoes I should add to the list, please let me know!
Atoms – Great reviews and an amazing story about the owner of the company
Bala Shoes – designed by nurses with consideration for structural differences in women’s feet
Casca Shoes – This is an interesting company that offers custom fit and a variety of options
New Balance Slip Resistant 626v2 work shoes
A note about high heels…
There is practically nothing worse for your feet than wearing high heels. (Sorry if you love them). If you wear them, please wear them only for special occasions and keep the heels as low as you can. If you are wearing heels in the hospital because it hurts to not wear heels, that’s a huge red flag and you need to really work on it.
Socks
When John Wooden, arguably the most famous coach in the NBA, starts the season by teaching his players how to put their socks on correctly, you can bet it’s important. Don’t skimp on socks. Buy good socks that fit well and take time to put them on correctly.
Compression socks have the potential to change your life. Ok, maybe that’s an exaggeration, but this is one thing I wish I had started earlier in my career. It’s not clear that they do anything to prevent the occupational hazard of varicose veins, but boy do they make your legs feel better at the end of a long day.
Make sure you throw an extra pair of socks in your call bag. There is nothing that feels better than taking your shoes and socks off after 10-12 hours, massaging and stretching your feet (if you have time) and putting on new socks before the second half of a 24 hour call. BTW, the same is true for shoes. Swapping out shoes (if you have two good pairs) is also really nice for your feet during a 24-hour call.
Foot stretching and massage – every day
A friend recently lent me this book which is written by Katy Bowman, with the help of 4 “goldeners” (all older than 70) about what they wish they’d known about caring for their physical wellbeing. Feet are literally the foundation of our musculoskeletal “chain” and unhealthy feet not only hurt, they can affect the function of your kness, hips, and back. Here is the routine recommended in the book to care for your feet. It only takes about 10 minutes and is something you will look forward to doing at the end of the day since it feels so good.
As an alternative, if you want a guided yoga practice for your feet, check out this video from the amazing Adrienne Mishler.
Pedicures and Ingrown Toenails
Every time you take a shower, look at your feet with intention. If you have calluses use a pumice stone to take off the layers of dead skin. Don’t let your toenails get out past the end of your toes and never cut them in a curve like you do your fingernails. If you start to get an ingrown toenail, soak your feet twice a day, dry them well, and then wiggle dental floss under the corners of the nail. Leave the dental floss in place until the next time you soak and then put another piece under the corner of the nail. Continue doing this until the nail grows out enough to be cut straight across. Since toenails grow about one millimeter a month, plan on it taking at least a month.
By the way, if you’ve never had a professional pedicure, ask around to find a good place and try it. It’s not just for women, so if you are a man who has never tried this, step out of your comfort zone (no pun intended) and try it at least once!
The Senn retractor is a small, relatively delicate retractor that is used extensively in hand surgery, vascular surgery, plastic surgery and other procedures involving the skin and soft tissue. I hold this instrument most days I am in the OR and yesterday found myself wondering about this beautiful tool.
Nicholas Senn was an early adopter of Listerism and performed his operations under a fog of carbolic acid spray. He felt that smooth surfaces on surgical instruments were important to help prevent infection.1 That, plus the need for retraction in superficial wounds undoubtedly led to developing the Senn retractor.
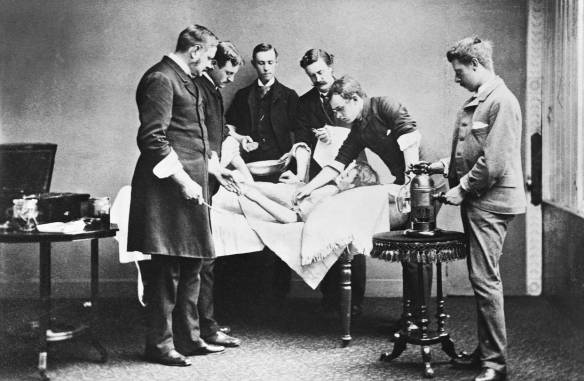 Surgery being performed under carbolic acid spray
Surgery being performed under carbolic acid spray
Nicolas Senn was born in 1844 and emigrated to the Fond du Lac, Wisconsin from St. Gaul, Switzerland in 1852. He graduated from Chicago Medical School in 1868, completed his residency at Cook County, started his academic career at the Medical College of Wisconsin, studied in Europe at the University of Munich and then returned as Professor at the University of Illinois. He served as president of the American Surgical Association in 1892, and was named president of the AMA in 19872, Dr.Senn was a military surgeon who served in the Spanish-American war and the Russo-Japanese war. Importantly, he founded the Association of Military Surgeons.2,3 He died in 1908 at the age of 64, five years before the American College of Surgeons was founded. There is little doubt that he would have been a founding member of the American College of Surgeons as he was the first Editor-In-Chief of SGO, which later became the Journal of the American College of Surgeons.4
In addition to his truly extraordinary resume, there are other facts and stories about Dr. Senn worth knowing. So, the next time you find yourself handing a student, resident, or assistant a Senn retractor you might want to share some of this history.
If you don’t work in an operating room, you may not be aware of the controversy going on about OR caps. To get right to the point – the surgeons think they should be allowed to wear the cloth hats they have worn forever. The Association of Operating Room Nurses (AORN) developed guidelines which included covering the ears and all hair (which means a bouffant paper hat). These guidelines were then implemented by JACHO which means they became “law” in every hospital in the United States.
 Anonymous surgeons demonstrating extremely effective covering of all hair with bouffant hats.
Anonymous surgeons demonstrating extremely effective covering of all hair with bouffant hats.
I’m a real believer in evidence based medicine (and policies) so I decided, like others, to look into what is really known about the issue. Because it is a conflict of interest, I need to disclose that I can’t stand the bouffant hats and I really, really miss my (clean and washed) cloth hats. (which BTW cover all my hair!)
What do the data say about the use of bouffant hats and infection rates?
Why don’t surgeons like bouffant hats?
It’s harder to keep them in place when wearing loupes or headlamps. If the goal is to keep the hair covered, this is a real problem. When moving headlamps, operating microscopes or loupes, the bouffant hat often moves substantially – or even comes off entirely.
They are hot. Many surgeons feel (me included) that the bouffant hats are uncomfortable and are hot. One can argue that anything that increases surgeon discomfort could affect concentration, which might be reflected in less focus on the operation.
Bouffant hats are expensive and bad for the environment. On Amazon, 100 bouffant hats cost $7.45. There were 48 million inpatient operations performed in 2009. When you add the 48 million outpatient procedures performed, that means there are roughly 100 million operations performed per year. (Mind you, these data are almost 10 years old, so it’s likely to be more now). If we assume an average of 4 cases/day by an average surgical team (nurses, CRNA, anesthesiologist, assistants/resident) and they all wear their hat for the day, the number of hats needed per year would be 100 million cases x 6 members of the team = 600 million hats/yr. 600 million hats divided by 100/box = 6 million boxes x $7.45 = $44,700, 000. Over 44 million dollars a year for the bouffant hats… all of which (600 million/year) end up in a land fill or are incinerated. p.s. Given that hats are often changed during the day, this number is probably on the low side.
It affects morale. In a survey of young (<45 years of age) surgeons, 71.2% stated that the new rules had affected surgeon morale.
They are inferior in blocking bacteria when compared to other caps. In a study of bouffant hats, disposable skull caps and cloth hats, the bouffant hat was the worst in preventing airborne bacterial contamination in the operating room. “I expect our findings may be used to inform surgical headgear policy in the United States,” he said. “Based on these experiments, surgeons should be allowed to wear either a bouffant hat or a skullcap, although cloth skull caps are the thickest and have the lowest permeability of the three types we tested.” Troy A. Markel, MD, FACS
I’m confident that in the very near future we will be back to wearing our clean, cloth hats. When you look at the data, and weigh the pros and cons, it seems pretty obvious what needs to be done….
Today I used an Allis clamp in the operating room. Like so many surgical instruments, it is a thing of beauty. It’s a balanced, well engineered tool designed to hold without crushing. And it has been used by surgeons all over the world since it was first first created.… in 1883.
Imagine if you will the operating room of 1883… it’s still the beginning of modern anesthesiology and the concept of antisepsis in surgery had been published by Lister less than 20 years before.
Surgeons in 1883 performed operations which were gory and painful. Patients routinely died, if not from the actual procedure then from the infections afterwards. Operating on the bowel in the 1880s was particularly dangerous with a mortality rate of 30-40%.
But despite the mortality (not to mention the morbidity and outright suffering), bowel obstructed by cancer or necrotic from strangulated hernias still needed to be resected. Faced with these outcomes and this suffering, surgeons in 1883, like we do now, studied, discussed, performed experiments and tried new techniques to improve the treatments they offered their patients. ( For a great review on the history of bowel anastomosis, click here.)
One of those surgeons was Oscar Huntington Allis.
Dr. Allis was born in 1836 in Holley, New York. He attended Jefferson Medical College and did an internship at the Philadelphia General Hospital. Like many surgeons of the era, he spent several years studying in Europe. Upon his return, he worked as a general surgeon at Presbyterian Hospital in Philadelphia. Dr. Allis died of a cerebral hemorrhage in 1921.
Here is Dr. Allis’ account of developing and using the Allis clamp (referred to as “toothed forceps”), which was delivered to the College of Physicians of Philadelphia in 1901. As you read this, remember that he was using a straight needle, much like a tailor would use.
My operation was performed in the following manner: If the reader will divest himself of his coat and place the cuffs parallel, he can look down into the sleeve ends as into a double-barrelled gun. The inner surfaces of the sleeves correspond to the mucous surfaces, and the outer surfaces to the serous surfaces of the gut ends. Now, if the reader will sew the two proximal edges of the coat sleeves together, by a suture that passes entirely through them, he will find that he can readily sew fully half their circumference together. If now he will turn in the remaining borders, he will find that he can readily complete the circuit by sewing the outer surfaces. It was precisely in this way that I finally successfully approximated the intestines in Case 2. The fact that the mucous membrane could be safely included in a suture emboldened me to repeat the operation; and finding by experience that my fingers could not always accomplish my purpose, I have added to my case two instruments that I have found very convenient not only as special aids in anastomoses, but also in general surgical work.
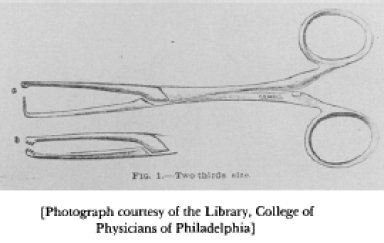 The first may be called tenaculum forceps (Fig. 1, a). I use them very much as women use pins and basting thread to secure their work temporarily while they are sewing it more securely. It does not matter what stitch is used–the whip stitch, through-and-through stitch, or over-and-over. All that is essential is that the approximated bowels should be securely united. Having firmly approximated one half the circumference, I remove the forceps, and, turning the partly united structures half round, I seize the seam with my tenaculum forceps, and with a pair basting the work a little further on (Fig. 3), the through-and-through suturing can be continued almost entirely around the entire circumference.
The first may be called tenaculum forceps (Fig. 1, a). I use them very much as women use pins and basting thread to secure their work temporarily while they are sewing it more securely. It does not matter what stitch is used–the whip stitch, through-and-through stitch, or over-and-over. All that is essential is that the approximated bowels should be securely united. Having firmly approximated one half the circumference, I remove the forceps, and, turning the partly united structures half round, I seize the seam with my tenaculum forceps, and with a pair basting the work a little further on (Fig. 3), the through-and-through suturing can be continued almost entirely around the entire circumference.
 When near the end of the approximation I have found toothed forceps (Fig. 1, b), with serrations on the edge, convenient for turning in the mucous edges, adjusting the serous, and holding them approximated until sutured (Fig. 4)
When near the end of the approximation I have found toothed forceps (Fig. 1, b), with serrations on the edge, convenient for turning in the mucous edges, adjusting the serous, and holding them approximated until sutured (Fig. 4)
At lunch last week with my clinical students the topic turned to which specialties they were considering for their future career. The senior resident (PGY6) on our service walked by and we asked her to join us. “Come sit down… we’re talking about how you choose a specialty.” She responded “You mean how a specialty chooses you.”
I believe that picking your specialty has far more in common with picking a spouse than anything else. All of us, at some point in our lives made a list of attributes we would like in our significant other… but… when we actually meet the person and fall in love, it’s almost a sure bet that who they are doesn’t really match the list… at least not entirely.
The wrong way to pick a specialty should be obvious – pick an “easy” specialty (or because the residency isn’t as demanding), or pick a specialty just because of what your income will be, or because it’s what you always said you would do. Just like picking who you will marry, choosing your specialty is not a choice that is made with lists of pros and cons. Some of the unhappiest doctors I know picked a residency because it was easy or because they thought the specialty would give them a better lifestyle… and then they were miserable because they hated the work.
Wear the White Coat
Almost every year I end up talking to a student who from the very first day of medical school was absolutely sure that he/she was going to be a surgeon. In choosing their rotations, they put surgery last – thinking that it would mean a better grade, better letters and a better chance for a good residency. They cruise through their other rotations superficially – interested enough to get decent evaluations and good grades – but never really engaged in the specialty. And then the unthinkable happens… they start their surgery rotation…. and they realize they don’t want to be a surgeon.
I tell students at the end of basic science that as they enter the clinics they should “wear the white coat”. When you are on pediatrics, be a pediatrician. When you are on internal medicine, be an internist. Don’t just think about it, try it on. When your attending asks you what field you are thinking about for your career, tell them that you are really interested in _____ (fill in the blank for the current rotation). It’s the truth…. you are interested. Show up every morning with the thought that this is the specialty you will be practicing the rest of your life. At the end of the rotation, you’ll have an honest understanding of the field… and you’ll be able to know for sure if it’s a good fit for you or not.
One other important thing to remember: there are more specialties out there than you will be exposed to…. The link below is the list of all boarded specialties in the United States.
http://www.abms.org/Who_We_Help/Physicians/specialties.aspx
Learn about specialties that sound interesting, meet physicians who practice them, and ask questions. You don’t have to be on a rotation to spend some time with a doctor in practice; most of them are delighted to have someone interested in the field spend some time with them. Email them and tell then you are interested and want to shadow them for a day or two.
How to Pick Your Specialty
I’ve watched the process enough to have a theory about how we pick our specialties. Here’s how I think it happens. The first thing that happens, as you go through your rotations, is you discover that you are more “medical” or “surgical”. I will warn you that it’s not predictable! Remember – somewhere over 70% of medical students end up in a field different from the one they predicted when they started medical school. The field of medicine needs both surgical and medical doctors. The two halves make up the whole, like the classic Yin-Yang symbol. And, like the symbol, every surgeon must have a little internist in them and vice versa if they are going to be a master in their field.
Once you are comfortable with your “medical” or “surgical” leanings, the next step is whether or not you want to care for the entire patient (e.g. general surgery, general medicine, family practice) or a part of the patient (e.g. ophthalmology, dermatology). Again, there is no judgment implied here – all the specialties are necessary and important. There’s one more branch in this decision tree… whether or not you want to work with children, adults or both. These are things you learn, not things you decide. I think my senior resident was absolutely right. The specialty chooses you. So how do you let it choose you? Listen. I don’t mean listen in the usual sense. Watch for the moments when you feel the tug to care for a certain kind of patient, notice when a role model makes the field seem appealing, pay attention when you get up in the morning and you can’t wait to get to the hospital. I don’t know of any better way to pick your specialty…. or let it pick you.